If someone breaks my leg, by accident or as a result of a fight, I can file a lawsuit. If someone breaks my heart (emotionally) I have no chance that justice will act on my behalf. Our Western society still follows Descartes. Mind and body are two independent organizations.
If I have cancer, I will surely arouse compassion and help, if I become depressed, I will be easily labelled as as a weak person who does not know or cannot face their reality. We have a vision of health and disease that has been typecast in concepts that have already expired. In the 21st century we must redefine health concepts.
“Health as the ability to adapt and self-manage, in light of the physical, emotional and social challenges of life”.
This new definition of health, developed and tested by Louis Bolk Institute researchers Machteld Huber and Marja van Vliet, marks a significant departure from the World Health Organisation’s definition of health. The latter defines health as ‘a state of complete physical, mental and social well-being and not merely the absence of disease or infirmity’. When this definition was coined in 1948, infectious diseases were the main problem. Today, however, chronic and lifestyle diseases are much more prevalent, particularly in the Western world.
The way in which ‘health’ is defined has a significant influence on how we organize and use health care. The requirement of ‘complete well-being’ in the WHO definition has unintentionally contributed to medicalisation: 95% of the present healthcare budget is spent on medication and intervention. Due to this focus, patients and healthcare providers often overlook other options for leading a high-quality, meaningful life with an illness.
The goal of today’s health care system is generally to bring people who are sick out of illness. This takes them from negative health to a state that is neutral—free from health problems but not necessarily thriving. Positive Health’s approach works with the positive—with what is right with you–—and builds on those assets to help achieve and maintain good health.
POSITIVE HEALTH
Positive Health is the scientific study of health assets. A “health asset” is a factor that produces stronger health, over and above risk factors for disease. Positive Health works to discover which specific health assets produce longer, healthy life, and which health assets lower disease risk and health care costs. The goal is to strive for optimal health —beyond the mere absence of illness.
Since 2008, the Positive Psychology Center of the University of Pennsylvania has undertaken a Positive Health initiative (Seligman, 2008). Critical to this is first defining what is meant by positive physical health. To this end, they have identified assets in three “psychological” domains that seem relevant to health: biological, subjective, and functional. A critical question is whether and how these assets promote health. Building on a considerable literature suggesting that negative psychological factors may increase the risk of cardiovascular disease (Everson and Lewis, 2005), they began by focusing on potential psychological assets in relation to cardiovascular outcomes.
The Positive Health initiative was inspired by the example of positive psychology (Peterson, 2006; Seligman, 2002; Seligman and Csikszentmihalyi, 2000). Until recently, mental health, like physical health, was usually understood to be the absence of mental illness (cf. Jahoda, 1958). Positive psychology challenged this assumption, arguing that mental health is real, consisting of a measurable configuration of positive emotions, engagement, good relationships, meaning, and accomplishment (PERMA: Seligman,2011). These states are by no means guaranteed by the mere absence or presence of mental illness. It’s been a couple of years since I signed up for a Positive Psychology online course by Professor Seligman at the University of Pennsylvania. By the way I approved it with “Honours”… As a psychologist I had an interest in this new line of research and I was excited by the methodology which convinced me the clinical evidence that was provided in the course. From my practice at a General Hospital, treating patients with physical ailments with significant emotional impact I was aware of the segmentation of the medicine. Body and mind as two offline worlds.
https://www.coursera.org/learn/positive-psychology-visionary-science/home/welcome
Later I followed the “Buddhism and Modern Psychology” course by Professor Robert Wright of Princeton University. Although different viewpoints coincide with the conclusions and evidence of Positive Psychology.
https://www.coursera.org/learn/science-of-meditation/home/welcome
In fact, thanks to clinical research we have made progress in diagnostics and therapeutics. In other words, we have made progress in treating physical or mental illnesses, but health in its self has not been sufficiently researched.
HEALTH ASSETS AND RESEARCH
Health assets are desirable, but research has clearly demonstrated the relevance of biological assets and suggested the importance of functional health assets to overall health. Still to be determined is whether and how subjective health assets contribute to health-related outcomes, including:
- Longevity
- Morbidity
- Quality-adjusted life years
- Prognosis when illness strikes
- Health care utilization and cost
Even less is known about the inter-relations between subjective, functional, and biological health assets.
IKIGAI
In this line we have a good example that health also depends on the “Reason for being” as we are taught by the Japanese from centuries ago with the Ikigai.
While there is no direct English translation, ikigai is thought to combine the Japanese words ikiru, meaning “to live”, and kai, meaning “the realization of what one hopes for”. Together these definitions create the concept of “a reason to live” or the idea of having a purpose in life.

https://www.weforum.org/agenda/2017/08/is-this-japanese-concept-the-secret-to-a-long-life/
Ikigai also has historic links: gai originates from the word kai, which means shell. These were considered very valuable during the Heian period (794 to 1185), according to Akihiro Hasegawa, a clinical psychologist and associate professor at Toyo Eiwa University, adding a sense of “value in living”.
To find this reason or purpose, experts recommend starting with four questions:
- What do you love?
- What are you good at?
- What does the world need from you?
- What can you get paid for?
NEXT STEPS IN POSITIVE HEALTH RESEARCH
Like positive psychology, Positive Health is, first and foremost, empirical. Therefore, we use the word“likely” because we are agnostic about what factors are actual health assets. There is a need to determine empirically which candidate health assets actually foster longer life, lower morbidity, lower health care utilization and cost, lower expenditures, better prognosis when illness does strike, and higher quality of life
Potential health assets that will be assessed through scientific research include levels of Vitamin D, body-mass index, optimism, ratio of “good” to “bad” cholesterol levels, stable marriage, exceptionally low blood pressure levels, meaningful work, and rapid wound healing, among others.
Additional research should examine the following relationships:
- Life satisfaction and heart disease
- Optimism and DNA sequence length
- Good social relationships and heart disease
- DNA sequence length and heart disease
- Psychological strengths and immunity
- Psychological strengths and heart function
- Exercise and heart disease
- Physical fitness and length of life
- Physical activity and obesity
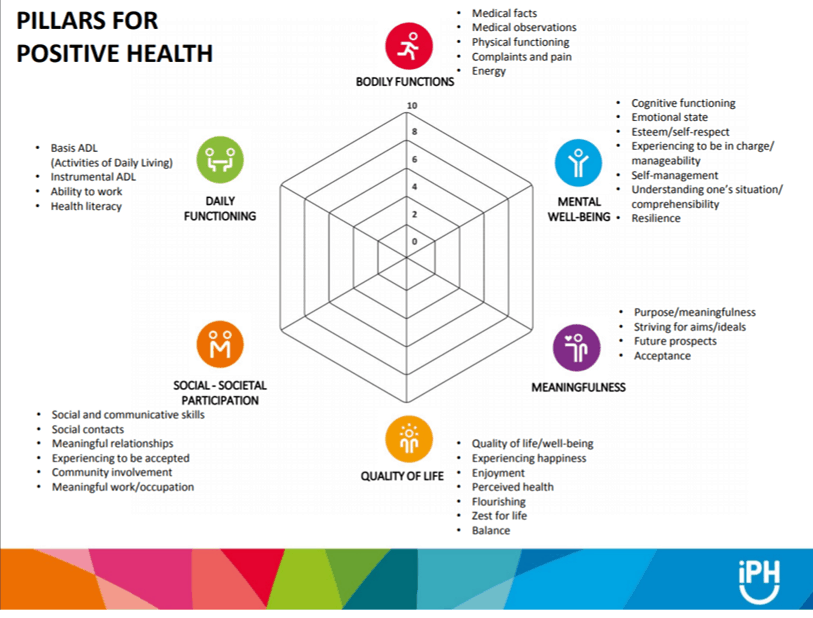
https://euprevent.eu/wp-content/uploads/2017/11/2.-Machteld-Huber-Positive-Health.pdf
Machteld Huber MD PhD. Institute Positive Health. Utrech
INNOLAB DIGITAL HEALTH DKV
A few weeks ago, in Barcelona, specifically in the BCN Health Hub, the InnoLab Digital Health DKV was presented. This initiative is part of the willingness to collaborate in the research and practice of what they announced as Smart Positive Health in words of Dr Julio Lorca who is the promoter of this initiative.
The InnoLab focus in four lines of digital health transformation:
- R&D for patient wellbeing and mental health
- Open innovation.
- Specialization in digital therapeutics
- Social impact and sustainability.
Congratulations !!!
SOURCES CONSULTED:
Preliminary evaluation of an adolescent positive health measurement scale: a salutogenic health promotion approach
https://journals.sagepub.com/doi/full/10.1177/1757975918757703
Positive affective processes underlie positive health behaviour change
https://www.tandfonline.com/doi/abs/10.1080/08870446.2017.1320798
Emotion, health decision making, and health behaviour
https://www.tandfonline.com/doi/full/10.1080/08870446.2017.1385787?src=recsys
The concept of Positive Health for students/lecturers in the Netherlands
https://www.tandfonline.com/doi/abs/10.1080/14635240.2019.1623707
Toward a model of positive health.
https://psycnet.apa.org/record/1989-40866-001
A causal model of positive health practices: the relationship between approach and replication.
https://psycnet.apa.org/record/1989-32552-001
Positive health
