We have experienced in recent years the adoption of Digital Technologies in our lives without just realizing it.This transformation is occurring in the health sector in a stealthier way, says Joan Cornet Prat, Board Member and Director of the Digital Health Observatory, ECHAlliance, Technical Engineer and Psychologist.
For example, the passage from traditional banking to online banking, the reservation of airline tickets or hotels for our vacations or access to music, movies or television series. It is a silent transformation.

Digital Therapeutics (TDx) is a new subsection of digital health that strives to directly deliver a therapy via use or interaction with software technology. The goal of Digital Therapeutics is to mirror an effective treatment and use technology to scale it to a larger patient population, thereby amplifying doctors’ and nurses’ care, changing patient behavior, and most importantly, reducing cost of care.

Source: Digital Therapeutics Alliance Report (1)
The term digital therapies appeared in 2013, in large part thanks to the CEO of Omada Health, Sean Duffy. He began using it at conferences and in the company’s promotional materials to describe his online coaching software aimed at helping Prediabetics avoid getting sick through exercise and weight loss.
An important step is the FDA (US) approving the first therapeutic digital prescription service
reSET® is the First Prescription Digital Therapeutic Cleared with Data Demonstrating Improved Outcomes of Abstinence and Treatment Retention in Patients with Substance Use Disorder (SUD) (2)
To support the FDA submission of reSET® (academic name: TES), a National Institute on Drug Abuse (NIDA) –sponsored clinical trial evaluated the therapeutic in 399 patients with SUD across 10 treatment centers in NIDA’s Clinical Trial Network nation-wide over 12 weeks. Patients were randomized to either a standard treatment-as-usual, which consisted of standard face-to-face counselling, or to a reduced amount of face-to-face counselling plus the digital therapeutic. The clinical study demonstrated that the digital therapeutic more than doubled the rate of abstinence compared to standard, face-to-face counselling. In a sub-group analysis of non-abstinent patients at study start, a poor prognostic indicator, patients randomized to the digital therapeutic demonstrated an almost five-fold improvement in abstinence.
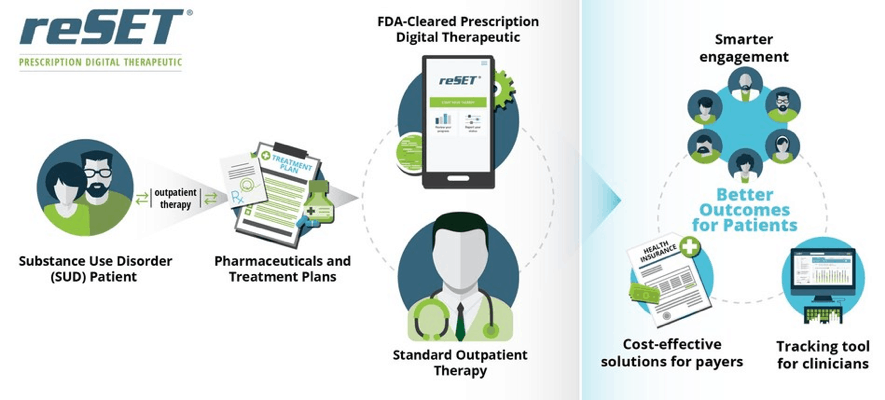
reSET® is intended to provide cognitive behavioral therapy, as an adjunct to a contingency management system, for patients 18 years of age and older who are currently enrolled in outpatient treatment under the supervision of a clinician. reSET® is indicated as a 12-week prescription-only treatment for patients with substance use disorder (SUD), who are not currently on opioid replacement therapy, who do not abuse alcohol solely, or who do not abuse opioids as their primary substance of abuse.
http://www.peartherapeutics.com
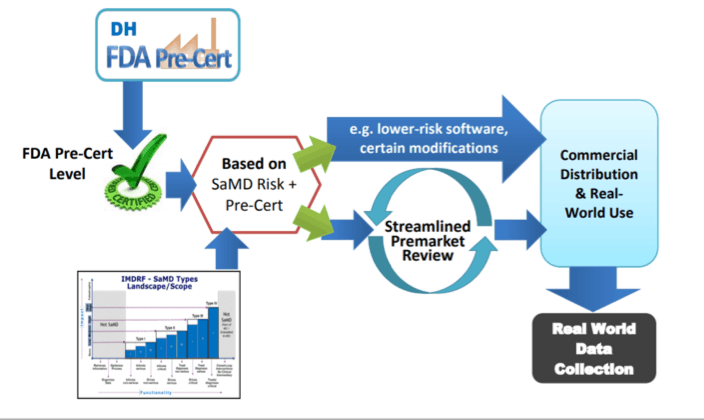 https://www.fda.gov/downloads/MedicalDevices/DigitalHealth/UCM568735.pdf
https://www.fda.gov/downloads/MedicalDevices/DigitalHealth/UCM568735.pdf
One of the objectives of Digital Therapeutics is the Patient Engagement to medical prescription. One of the greatest challenges in the treatment of patients with chronic illnesses is the follow-up of their therapeutic guidelines, especially when it comes to multiple diseases. With the contribution of digital technologies opens a great opportunity not only for the improvement of the health and quality of life of the patient but also for projects of Big Data in health research.
European Union is speeding up Digital Therapeutics.
In Europe there is a new and ambitious Project that is in its beginnings- PARADIGM. “Patients Active in Research And Dialogues for an Improved Generation of Medicines: Advancing meaningful patient engagement in the life cycle of medicines for better health outcomes” financed in part by The European Union within the framework of Innovative Medicines Initiative 2 and coordinated by the FORUM EUROPEAN DES PATIENTS (FPE) with numerous industry and pharma partners , hospitals and patient associations. (3)
PARADIGM will develop a strategy for sustaining the long-term implementation of Patient Engagement (PE) resources aimed at structuring and supporting the community. This will be a game-changer, addressing fundamental gaps and creating real assets to ensure the sustainability of the PE ecosystem in the years to come.
PARADIGM has a common vision and values-base, and is a highly innovative, consensus-oriented, and experienced consortium, comprising pan-European leaders in patient engagement, academia, SMEs, health professionals, pharmaceutical and biotech companies, pharmaceutical corporate associations, and representatives of competent authorities, all bringing complementary know-how to partner with industry, and a strong commitment to transform patient engagement in Europe.
Mental Health leading the race…
A team of researchers from different Australian, British and American institutions is convinced that depression can be effectively combated through the use of certain smartphone applications. In a study published in World Psychiatry magazine, these experts point out that this type of computer tools will allow many people to deal with this mental disorder that, according to the World Health Organization, affects more than 300 million individuals.
In his essay – The first of its kind to take place – coordinated by Joseph Firth of the Australian National Institute of Complementary Medicine (NICM) and the Department of Psychology and Mental Health at the University of Manchester, the specialists have had in Account 22 mobile applications developed by professionals to make clinical trials – including MoodHacker, MyCompass, Get Happy, IBobbly… – and data from 3,400 men and women between 18 and 59 years who had been diagnosed with different types of Illnesses or mental conditions, from the aforementioned depression or bipolar disorder, to anxiety or insomnia.
Thus, they have been able to determine that, in general, these types of interventions managed to significantly reduce the symptoms related to depression, which, in the opinion of Firth and its collaborators, suggests that these digital therapies can be very useful for many, especially those who are not able to access another type of treatment. (4)
Digital Therapeutics in the Landscape of Digital Health solutions
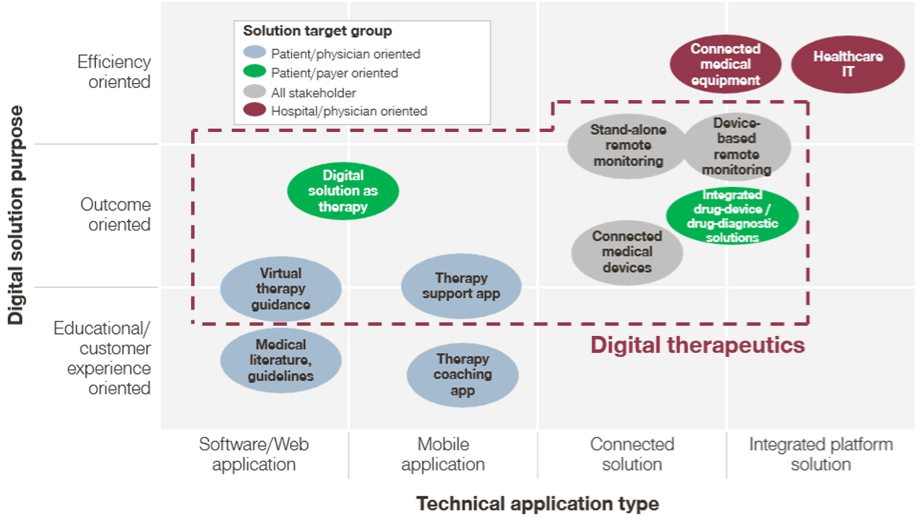 https://www.simon-kucher.com/en/blog/monetizing-digital-therapeutics
https://www.simon-kucher.com/en/blog/monetizing-digital-therapeutics
The orientation to the treatment of diseases and the development of prescription products are two of the characteristics of these companies that equate them with traditional pharmaceuticals.
Putting in the point of view the therapeutic efficacy on specific clinical outcomes represents, without doubt, a remarkable leap for mobile health and digital health applications in general, but it is still early to know how far these digital therapies (digital therapeutics or “digiceuticals”, as they are called in the jargon of the sector) can be as effective as the drugs or even deserve the denomination of therapy. The path undertaken to demonstrate its efficacy through clinical trials certainly points towards convergence, but there are still many steps left until these therapies enter the routine of physicians and patients, and their benefits and possible side effects and adverse reactions.
Digital Therapeutics, what do they mean for pharma firms?
As payers become more focused on Value Based Contracts (VBCs), the days of pay-per-pill are disappearing. Drugs will remain core but they will be augmented by a portfolio of digital therapies, wrap-around services and data analytics, which providers will pay for according to overall patient outcomes.
Digital therapeutics (DTx) deliver evidence-based therapeutic interventions to patients that are driven by high quality software programs to prevent, manage, or treat a medical disorder or disease. They are used independently or in concert with medications, devices, or other therapies to optimize patient care and health outcomes.
DTx products incorporate advanced technology best practices relating to design, clinical validation, usability, and data security. They are validated by regulatory bodies as required to support product claims regarding risk, efficacy, and intended use.
A new road to improve the benefit of all health stakeholders?
Digital therapeutics empower patients, healthcare providers, and payers with intelligent and accessible tools for addressing a wide range of conditions through high quality, safe, and effective data-driven interventions.
What is the value of digital therapeutics?
Individual digital therapeutics have the potential to:
- Enhance and support current medical treatments
- Provide patients, providers, and payers with novel therapy options for unmet medical needs
- Be used independently or in conjunction with other therapies
- Reduce reliance on certain pharmaceuticals or other therapies
- Integrate into medical guidelines and best practices
DTx tend to fall into three groups.
- Developers and mental health researchers have built digital solutions which typically provide a form of software delivered Cognitive-Behaviour Therapies (CBT) that help patients change behaviours and develop coping strategies around their condition.
- The group of Digital Therapeutics which target lifestyle issues, such as diet, exercise and stress, that are associated with chronic conditions, and work by offering personalised support for goal setting and target achievement.
- DTx designed to work in combination with existing medication or treatments, helping patients manage their therapies and focus on ensuring the therapy delivers the best outcomes possible.
Like all medical therapies, digital therapeutics must pass the bar of being clinically validated in rigorously designed and peer-reviewed studies.
References
- Digital Therapeutics: Combining Technology and Evidence-based Medicine to Transform Personalized Patient Care (https://www.dtxalliance.org/wp-content/uploads/2018/09/DTA-Report_DTx-Industry-Foundations.pdf)
- Pear Therapeutics Obtains FDA Clearance of the First Prescription Digital Therapeutic to Treat Disease (https://www.prnewswire.com/news-releases/pear-therapeutics-obtains-fda-clearance-of-the-first-prescription-digital-therapeutic-to-treat-disease-300520068.html)
- Patients Active in Research and Dialogues for an Improved Generation of Medicines: Advancing meaningful patient engagement in the life cycle of medicines for better health outcomes: https://cordis.europa.eu/project/rcn/216092/factsheet/en
- Firth, J. , Torous, J. , Nicholas, J. , Carney, R. , Pratap, A. , Rosenbaum, S. and Sarris, J. (2017), The efficacy of smartphone‐based mental health interventions for depressive symptoms: a meta‐analysis of randomized controlled trials. World Psychiatry, 16: 287-298. doi:10.1002/wps.20472: https://onlinelibrary.wiley.com/doi/full/10.1002/wps.20472
Sources consulted:
- Explore How Digital Therapeutics Boost Medical Workflow and Patient Communications: https://en.prnasia.com/releases/apac/explore-how-digital-therapeutics-boost-medical-workflow-and-patient-communications-213797.shtml
- A randomized, controlled pilot trial of the Emotional Faces Memory Task: a digital therapeutic for depression: https://www.nature.com/articles/s41746-018-0025-5
- Digital Therapeutics Alliance: https://www.dtxalliance.org/
- Exploring the potential of digital therapeutics: https://www.mckinsey.com/industries/pharmaceuticals-and-medical-products/our-insights/exploring-the-potential-of-digital-therapeutics
- Digital therapeutics: Preparing for takeoff: https://www.mckinsey.com/industries/pharmaceuticals-and-medical-products/our-insights/digital-therapeutics-preparing-for-takeoff
- Digital Health Innovation Action Plan. FDA: https://www.fda.gov/downloads/MedicalDevices/DigitalHealth/UCM568735.pdf
